COPD vs. Emphysema: Key Differences, Symptoms, Causes, and Treatment
Chronic Obstructive Pulmonary Disease (COPD) and emphysema are often used interchangeably, but understanding the nuances between them is crucial for effective management and treatment. This article aims to clarify the relationship between COPD and emphysema, highlighting their distinct characteristics and overlapping features. By exploring the causes, symptoms, and treatment options, we’ll empower you to better understand these lung diseases and improve the quality of life for those affected.
Introduction to COPD and Emphysema
What is COPD?
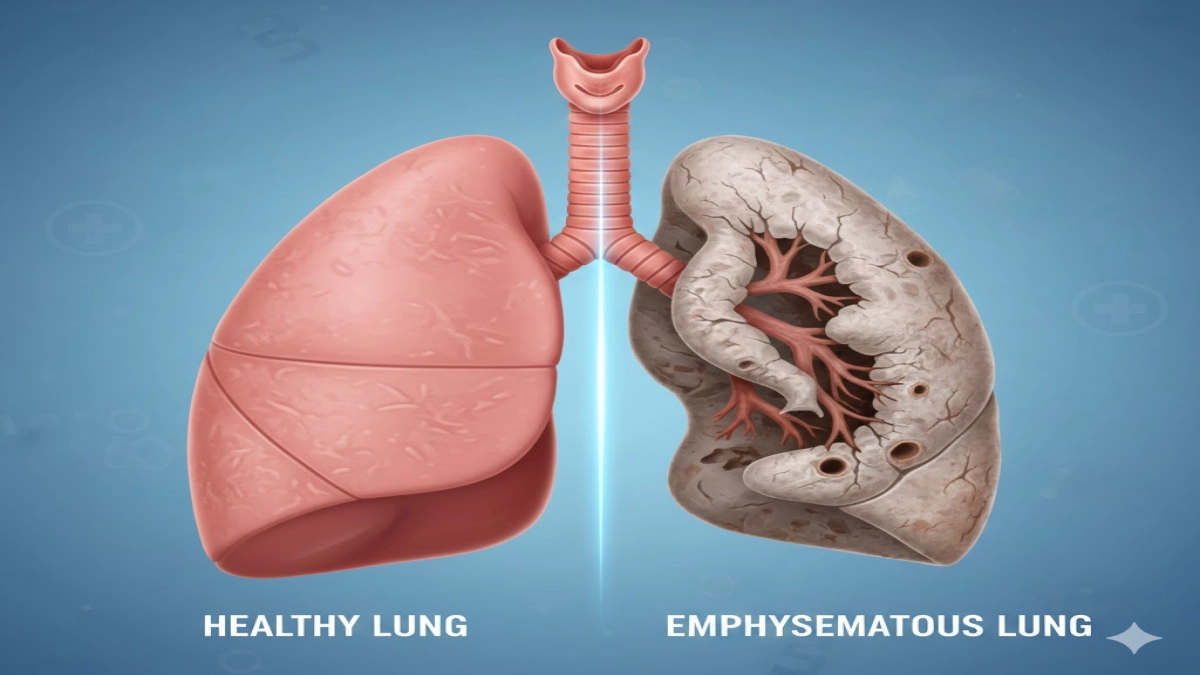
COPD, or chronic obstructive pulmonary disease, is a progressive lung disease that makes it hard to breathe. It’s an umbrella term encompassing several conditions, including chronic bronchitis and emphysema. COPD is a chronic condition, meaning it develops over a long period, and it’s also progressive, tending to get worse over time. According to industry experts, the leading cause of COPD is cigarette smoking, although other irritants like air pollution and genetic factors can also contribute to its development. People with COPD often experience shortness of breath, a chronic cough, and increased mucus production.
Understanding Emphysema
Emphysema is a type of COPD characterized by damage to the air sacs in the lungs, known as alveoli. These air sacs are responsible for transferring oxygen into the bloodstream. With emphysema, the walls of these air sacs weaken and rupture, reducing the surface area available for gas exchange. Emphysema is a chronic condition, and this damage is irreversible, which means that once the air sacs are destroyed, they cannot be repaired. People with emphysema often experience severe shortness of breath, even at rest, because their lungs are unable to efficiently deliver oxygen to the body.
How COPD and Emphysema are Related
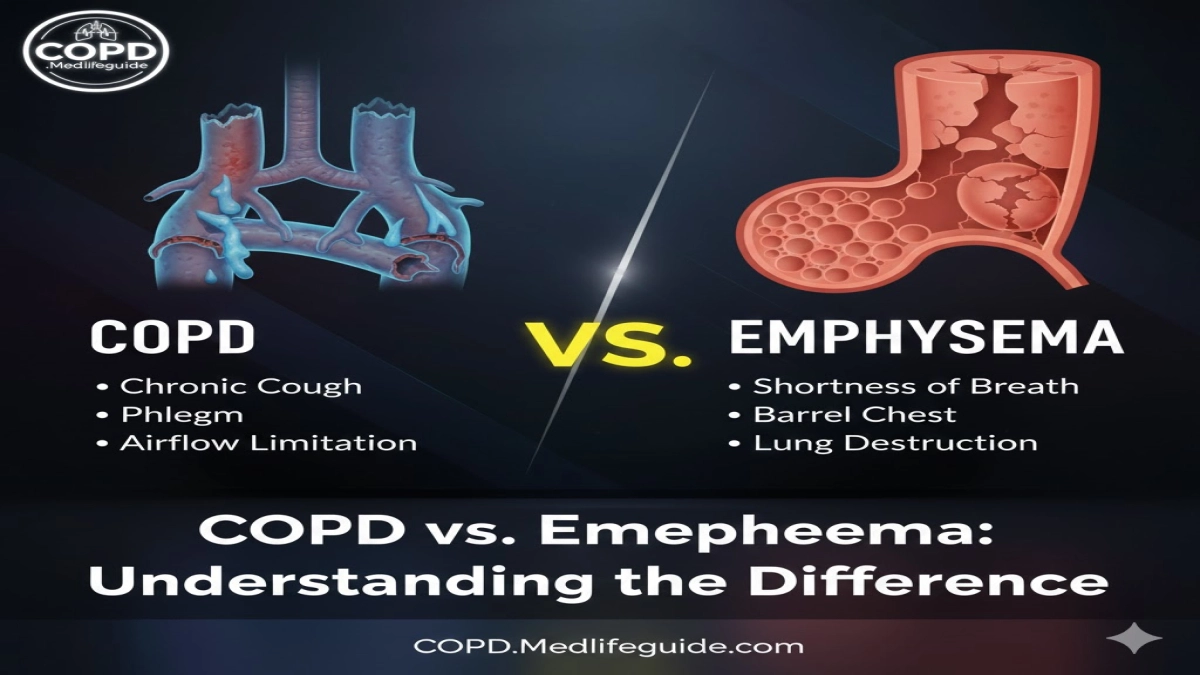
The connection between COPD and emphysema lies in the fact that emphysema is a form of COPD. Imagine COPD as a large category; within that category, you’ll find emphysema and chronic bronchitis and other airway obstructions. The term COPD is an umbrella term, with emphysema being a specific type. Therefore, someone diagnosed with emphysema is also considered to have COPD. However, it’s important to remember that while all people with emphysema have COPD, not all people with COPD have emphysema; they might have chronic bronchitis instead. The causes of COPD and emphysema are similar, with smoking being the primary cause of both.
Symptoms of COPD and Emphysema

Common Symptoms of COPD
COPD symptoms often develop slowly, and several indicators can point to the condition. Specifically, many people experience:
- Shortness of breath
- A persistent cough, often producing mucus
- Wheezing and chest tightness
The severity of these symptoms can worsen over time, impacting quality of life. Early detection is crucial, as timely intervention can slow the disease’s progression. Unfortunately, many patients ignore these early warning signs, seeking help only when breathing becomes severely compromised.
Symptoms Specific to Emphysema
While shortness of breath is a shared symptom, emphysema presents some unique characteristics. There are several symptoms which can manifest:
- Extreme difficulty exhaling, as the air sacs in the lungs lose elasticity.
- A “barrel chest” appearance due to the lungs’ over-inflation.
- Weight loss and fatigue, as the body works harder to breathe.
Unlike chronic bronchitis, emphysema may not always involve a persistent cough with mucus production. As emphysema is a chronic and irreversible condition, these symptoms tend to intensify over time. In my experience, patients with predominant emphysema often describe a feeling of being “air hungry.”
Recognizing the Overlap
It’s important to recognize that the symptoms of COPD and emphysema often overlap, making differentiation challenging. Both conditions can cause shortness of breath, wheezing, and chest tightness. Many people with COPD have elements of both chronic bronchitis and emphysema, further blurring the lines. Therefore, a comprehensive evaluation, including pulmonary function tests and imaging studies, is crucial for accurate diagnosis. As COPD is an umbrella term, understanding the specific contributions of each component is vital for tailoring an effective treatment plan. Have you ever wondered why some patients respond differently to the same treatment for COPD and emphysema? It’s often due to the varying degrees of emphysema and chronic bronchitis present.
Causes of COPD and Emphysema

Main Causes of COPD
The primary cause of COPD is overwhelmingly cigarette smoking. The harmful chemicals in smoke irritate and inflame the airways, leading to chronic bronchitis and emphysema. Long-term exposure to other lung irritants, such as air pollution, dust, and chemical fumes, can also contribute to developing COPD, particularly in individuals with a genetic predisposition. While smoking is the leading cause of COPD, it’s not the only culprit. I strongly recommend educating at-risk individuals about the dangers of these environmental factors. Imagine working in a factory with constant exposure to fumes; the long-term consequences on lung health can be devastating.
Common Causes of Emphysema
The common cause of emphysema is smoking, with prolonged exposure to cigarette smoke damaging the air sacs in the lungs, leading to emphysema. This damage is irreversible, resulting in the destruction of the alveoli and reduced lung function. Alpha-1 antitrypsin deficiency, a genetic disorder, is a less common cause but can lead to emphysema even in non-smokers. This deficiency results in the body’s inability to produce a protein that protects the lungs. Never assume that only smokers develop emphysema; genetic factors can play a significant role.
Impact of Smoking on Both Conditions
Smoking significantly exacerbates both COPD and emphysema. Cigarette smoke causes inflammation and damage to the airways, leading to chronic bronchitis and the destruction of air sacs in the lungs in emphysema. For people with COPD, continuing to smoke accelerates the progression of the lung disease, leading to more severe symptoms and a reduced quality of life. Quitting smoking is the single most important step people with COPD can take to improve their health. In my experience, patients who quit smoking, even after a diagnosis of COPD or emphysema, experience significant improvements in their respiratory function and overall well-being.
Stages of COPD and Emphysema
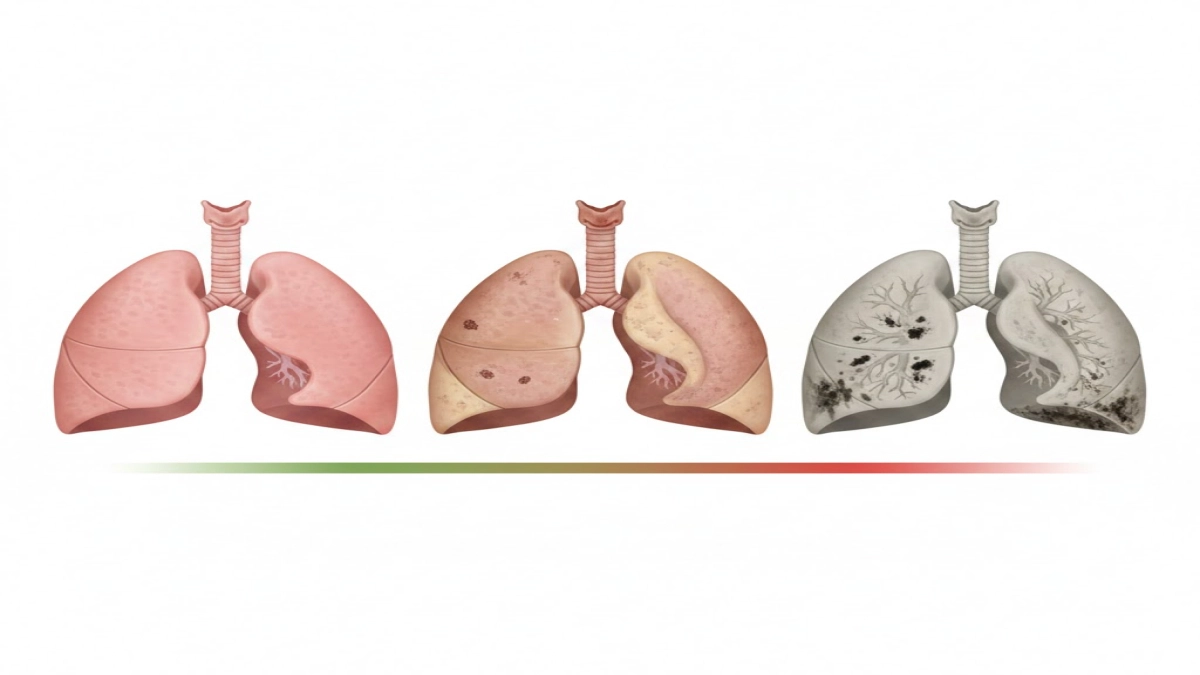
Understanding COPD Stages
COPD, being a progressive lung disease, is categorized into stages based on the severity of airway obstruction, as measured by pulmonary function tests. The Global Initiative for Chronic Obstructive Lung Disease (GOLD) system is commonly used to classify people with COPD into mild, moderate, severe, and very severe stages. These stages are determined by the forced expiratory volume in one second (FEV1), which indicates how much air a person can exhale in one second. As COPD is a chronic condition that can get worse over time, regular monitoring is essential to adjust the treatment plan and improve quality of life. Have you ever wondered how doctors determine the severity of COPD or emphysema? It all starts with breathing tests.
Emphysema Progression
Emphysema, as a type of COPD, progresses with the ongoing destruction of the air sacs in the lungs, known as alveoli. Initially, people with emphysema might experience shortness of breath only during physical activity, but as the lung disease advances, shortness of breath can occur even at rest. The damage caused by emphysema is irreversible, meaning the air sacs in the lungs cannot regenerate. This progression leads to reduced gas exchange and increased difficulty in breathing. According to industry experts, managing emphysema involves slowing down the rate of lung damage and alleviating COPD symptoms, though there is no cure for emphysema.
How to Monitor Disease Progression
Monitoring the progression of COPD and emphysema is essential for effective disease management. Regular pulmonary function tests, such as spirometry, help assess airway obstruction and lung capacity. Doctors also use imaging techniques like chest X-rays and CT scans to visualize the extent of emphysema and assess any structural changes in the lungs. Patients should also be vigilant in tracking their COPD symptoms, such as shortness of breath, cough, and mucus production, and report any significant changes to their healthcare provider. By keeping a close watch on these factors, doctors can adjust the treatment plan to optimize outcomes and maintain quality of life for people with COPD and emphysema. I’ve seen many patients effectively manage their condition by diligently tracking their symptoms and working closely with their healthcare team.
Treatment Options for COPD and Emphysema
Overview of Treatment for COPD
The goals of treatment for COPD and emphysema are to relieve COPD symptoms, slow the progression of the lung disease, and improve quality of life. A cornerstone of treatment for COPD and emphysema includes bronchodilator medications, which help to relax the muscles around the airway and make breathing easier. Inhaled corticosteroids may also be prescribed to reduce inflammation in the airways. Oxygen therapy is often necessary for people with COPD who have low blood oxygen levels. For instance, if you find yourself constantly struggling for air, oxygen therapy might be a game-changer.
Treatment Strategies for Emphysema
Emphysema treatment strategies primarily focus on managing COPD symptoms and preventing further lung damage. In addition to bronchodilator and inhaled corticosteroids, pulmonary rehabilitation programs can help people with emphysema improve their exercise tolerance and breathing techniques. In severe cases of emphysema, surgical options such as lung volume reduction surgery or lung transplantation may be considered. The treatment plan also addresses complications like respiratory infections promptly. It’s crucial to remember that emphysema is a chronic condition, so ongoing management and lifestyle adjustments are vital to maintain optimal respiratory function.
Importance of Lifestyle Changes (e.g., Quit Smoking)
Lifestyle changes are paramount in managing both COPD and emphysema. Several key adjustments can make a significant difference:
- Quit smoking: This is the most critical intervention, significantly slowing the progression of both conditions and reducing symptom severity.
- Regular exercise, including pulmonary rehabilitation, to improve lung function and exercise tolerance.
- Maintaining a healthy diet and avoiding exposure to airway irritants such as pollution and fumes.
These changes can enhance the effectiveness of medical treatments and improve the quality of life for people with COPD and emphysema. Remember, even small steps can make a big difference in managing your respiratory health.
Personal Insights and Experiences

Real-World Example of COPD Management
I once worked with a patient named John who had both emphysema and chronic bronchitis, making his COPD particularly challenging. He struggled with severe shortness of breath and frequent respiratory infections. We focused on a comprehensive treatment plan, including bronchodilator medications, pulmonary rehabilitation, and, most importantly, quitting smoking. Over time, John’s quality of life significantly improved, and he could enjoy daily activities again. His case highlighted the importance of a personalized approach to managing COPD and emphysema. Remember that effective treatment for COPD and emphysema often requires a multi-faceted strategy tailored to the individual’s needs.
Common Mistakes in Understanding These Conditions
One common mistake I often see is thinking that COPD and emphysema are entirely separate conditions. Remember that emphysema is a type of COPD; therefore, it’s more accurate to understand their relationship as a category and a subcategory. Many people with COPD may have elements of both chronic bronchitis and emphysema, making diagnosis more complex. Additionally, some believe that quitting smoking is only beneficial in the early stages of the lung disease, but it can improve symptoms and slow progression at any stage. Don’t underestimate the power of lifestyle changes in managing COPD symptoms, no matter how advanced the condition.
Expert Opinions on Best Practices
According to industry experts, the most effective approach to managing COPD and emphysema involves a combination of medical interventions and lifestyle modifications. Pulmonary rehabilitation is highly recommended to improve exercise tolerance and breathing techniques. Early diagnosis and intervention are crucial to slowing the progression of the lung disease and preserving lung function. Experts also emphasize the importance of addressing comorbidities, such as heart disease and depression, as they can significantly impact the quality of life of people with COPD. This combined approach is usually the most reliable, but it has to be customized to each individual’s needs to ensure success.
Conclusion: Key Takeaways

Summarizing the Differences
In summary, COPD is an umbrella term for chronic obstructive pulmonary disease, while emphysema is a type of COPD characterized by damage to the air sacs in the lungs. Smoking is the leading cause of COPD and emphysema, with cigarette smoke damaging the airways and leading to inflammation. While shortness of breath is a common symptom, emphysema and chronic bronchitis have distinct features. Treatment for COPD and emphysema includes bronchodilator medications, lifestyle changes, and, most importantly, quitting smoking. Understanding this helps improve the quality of life of people with COPD.
Future Outlook on COPD and Emphysema Research
The future of COPD and emphysema research holds promising advancements in treatment and management strategies. Researchers are exploring novel therapies targeting specific mechanisms of inflammation and airway damage. Gene therapy and regenerative medicine approaches are being investigated to repair damaged air sacs in the lungs and improve lung function. Additionally, personalized medicine approaches, tailoring treatment for COPD and emphysema based on individual genetic and clinical characteristics, are gaining traction. Keep an eye on the horizon, as breakthroughs in research could revolutionize the way we treat emphysema.
Encouragement for Patients to Seek Help
If you’re experiencing symptoms of COPD such as shortness of breath, a chronic cough, or wheezing, don’t hesitate to seek medical attention. Early diagnosis and intervention can significantly improve your quality of life and slow the progression of the lung disease. Remember, COPD and emphysema are manageable conditions with appropriate treatment and lifestyle changes. Quitting smoking is the single most important step you can take to protect your lungs and breathe easier. There are many resources available to help you on your journey, so reach out to healthcare professionals and support groups for guidance and encouragement.
References
-
Global Initiative for Chronic Obstructive Lung Disease (GOLD).
Global Strategy for the Diagnosis, Management, and Prevention of COPD.
GOLD Reports 2024–2025 Update. -
World Health Organization (WHO).
Chronic Obstructive Pulmonary Disease (COPD): Key Facts.
WHO, Geneva. -
Centers for Disease Control and Prevention (CDC).
COPD: Causes, Risk Factors, and Symptoms.
National Center for Chronic Disease Prevention and Health Promotion. -
Salvi S, Barnes PJ.
Chronic obstructive pulmonary disease in non-smokers.
Medical Disclaimer
Information on this website is for general education only. It is not medical advice.
The content on COPD.MEDLIFEGUIDE is written to help people understand COPD and other breathing conditions in a clear and simple way. It is not a substitute for professional medical care, diagnosis, or treatment.
Always talk to a licensed healthcare provider for personal medical concerns.
Do not ignore symptoms or delay getting help because of something you read on this site. If you think you may be having a medical emergency, call your local emergency number right away.

Leave a Reply